Community-Acquired Pneumonia (CAP)
October 2019 IDSA CAP Adult Guidelines / CHEST CAP in Immunocompromised Patients / IDSA CAP in Kids Guidelines / 2025 Diagnosis and Management of Community-acquired Pneumonia. An Official American Thoracic Society Clinical Practice Guideline
CAP is defined as pneumonia with an onset outside of the hospital setting or < 48 hours after hospital admission. Mortality ranges from < 1% to 50% depending on severity of illness. It is one of the leading infectious causes of hospitalization and
death.
Bacterial CAP is usually caused by S. pneumonia, H. influenza, S. aureus, legionella (usually more severe), mycoplasma and Chlamydophila (less severe), and pseudomonas and Enterobacteriaceae sometimes isolated.
Etiology:
| Unidentified (55-74%) | Viral (14-27%) | Bacterial (15-29%) |
| Presumed infection, but no pathogen identified (or no cultures) | Rhinovirus 3‐13% Influenza 1‐6% Human metapneumovirus 1‐4% Coronavirusa 2‐3% Parainfluenza 2‐3% Respiratory syncytial virus 1‐3% Other 2% | Streptococcus pneumoniae 5‐14% Staphylococcus aureus 1‐5% Haemophilus influenzae <1‐6% Mycoplasma pneumoniae 1‐3% Pseudomonas aeruginosa <1‐3% Legionella spp. 1% Other 3‐5% |
You don’t usually do cultures in CAP unless it’s severe CAP or if Legionella is suspected. Chest infiltrate and cough/sputum are diagnostic. If hospitalized/severe, you want to get gram stain, sputum cultures, blood cultures *2. You may also get MRSA nares, pneumococcal and Legionella urinary antigens, , Don’t go by procalcitonin to diagnose or to discontinue therapy (more on procal further down).
For CAP, there are a few “scores” you should be familiar with. The CURB-65 has fallen out of favor, but it’s quick and easy and still may be tested. However, we usually don’t use it to determine ICU admission anymore (I left that in because some practitioners still do), it’s sometimes used for inpatient vs outpatient. To determine whether to admit to ICU or the floor, you should use clinical criteria and provider judgment.
- 1 point each: Confusion, Urea >19, Respiratory Rate >=30, Blood pressure <90 SBP or <=60 DBP, age >=65
- Score = 0 or 1: can treat as outpatient
- Score = 1: consider admission, but can closely watch as outpatient
- Score = 2: Inpatient admission, consider ICU
Generally, the Pneumonia Severity Index is preferred, but it’s far more complicated. It predicts patients who can be treated as outpatients better, saving unnecessary hospitalizations. A tool or scorecard must be used to obtain this score.
- <=70 outpatient
- 71-90-Inpatient observation
- >=91-Admission
DRIP Scores
Another score you’ll sometimes see in relation to CAP is the DRIP (Drug Resistance in Pneumonia) score. This is used to predict a patient’s probability of having a resistance infection. This can help with adding pseudomonal coverage. A patient with a DRIP score <4 can be treated effectively without broad-spectrum antibiotic coverage, while a patient with a score ≥4 is more likely to require broad- spectrum antibiotic coverage. The DRIP score is more predictive than the healthcare-associated pneumonia (HCAP) criteria were for drug-resistant pathogens, and may have the potential to decrease antibiotic overutilization in pneumonia (Webb BJ, Sorensen J, Mecham I, et al. Antibiotic use and outcomes after implementation of the drug resistance in pneumonia score in ED patients with community-onset pneumonia. Chest. 2019;156(5):843-851.).
You can use an online calculator. It considers antibiotic use, prior diagnoses, long-term care residency, and other minor factors.
IDSA criteria for severe CAP
| Criteria | Severe | ICU? |
| Major Criteria: Septic shock requiring vasopressors Respiratory failure requiring mechanical ventilation | >=1 Major | Yes |
| Minor Criteria: Respiratory rate > 30 breaths/min PaO2/FiO2 ratio < 250 Multilobar infiltrates Confusion/disorientation Uremia (blood urea nitrogen level > 20 mg/dL) Leukopeniaa (white blood cell count < 4000 cells/mL) Thrombocytopenia (platelet count < 100,000/mL) Hypothermia (core temperature < 36C) Hypotension requiring aggressive fluid resuscitation | >-3 minor | Maybe |
For the ATS 2025 Guideline: severe community-acquired pneumonia was defined as CAP requiring mechanical ventilation or vasopressors, or with three “minor criteria” (e.g., tachypnea >30 breaths/minute, P/F ratio <250, or various “SIRS/sepsis” criteria.
Other Diagnosis:
- Lung ultrasound as an acceptable alternative to chest x-ray in skilled settings according to the new ATS guidelines.
- Respiratory panels can narrow therapy quickly, and sometimes can replace sputum cultures
- Note that the new ATS guidelines suggest empiric abx for patients with resp virus if the patient is inpatient or has comorbidities
Outpatient treatment:
- No comorbidities: Amoxicillin TID
- Can use doxycycline 100 mg every 12 hours
- Macrolide only if above are contraindicated AND local resistance <25%
- There is some controversy over the above suggestion as Amoxicillin has poor sensitivity against MSSA in most areas, and has no coverage over Mycoplasma pneumonia, or Moraxella catarrhalis, some of the top causes of CAP. Many clinicians use Augmentin or add/or a macrolide.
- Comorbities: B-lactam (Augmentin, Cefpodoxime, Cefuroxime) PLUS macrolide or doxycyline
- Can use levofloxacin or moxifloxacin (“respiratory fluoroquinolones”)
- *Consider MRSA if IV antibiotics in last 90 days or pseudo/MRSA in last year
- According to the guidelines, duration of therapy should be ≥ 5 days for all regimens, after which the patient’s vital signs, ability to eat, and mentation should be evaluated to ensure recovery. Recent evidence has show treatment courses as short as 3-5 days may be sufficient in some patients.
- Comorbidities: alcoholism, asplenia, diabetes, malignancy, chronic heart, lung, liver or kidney disease.
Inpatient Treatment:
- No comorbidities: B-lactam (usually Unasyn, cefotaxime, ceftaroline, ceftriaxone) PLUS macrolide or doxycyline
- Can use levofloxacin or moxifloxacin
- If prior MRSA (1 year): add vanc or linezolid
- If prior pseudo (1 year): add cefepime, pip-tazo, ceftazidime, imipenem, meropenem or aztreonam
- If prior hosp. and IV antibiotics or locally validated resistance factors: add drugs after cultures
- Comorbidities: CHF, lung, liver, renal disease, diabetes, alcoholism, malignancies, asplenia, immunosuppression, antimicrobial in past 3 months
- Severe: B lactam plus either a macrolide or flouroquinolone. No flouroquinolone alone
- Add on as above
- Severe is: septic shock, respiratory failure/ventilation or 3 of: rr > 30 breaths, PaO2/FI02<250, multilobar infiltrates, confusion, uremia (>20), leukopenia (<4000), thrombocytopenia (<100,000), hypothermia or hypotension requiring aggressive resuscitation
- Controversy: Many argue that there aren’t many places where a fluoroquinolone PLUS a macrolide would be preferred. A fluoroquinolone plus azithromycin makes more sense, but it is not guideline-indicated but this guideline is supported by weak evidence. In most cases, a fluoroquinolone alone would likely work when the patient is not able to take a beta-lactam.
- Deescalate 48 hours after cultures or MRSA swab
- Do not add routinely add anaerobic coverage for aspiration.
- Give all CAP patients with flu Tamiflu, no matter how long they’ve had flu symptoms
- Duration: continue until clinically stable, minimum of 5 days, 7 days if suspected MRSA or pseudo. Serial procalcitonin can support discontinuation. If 80% drop, may DC (see procal section below). New ATS guidelines state: Less than five days of antibiotics (minimum of 3 days) for outpatients, five or more days of antibiotics for inpatients.
- Exclusions for shorter therapy: immunocompromised patient (neutropenia, asplenia, substantial cirrhosis), bacteremia (usually will need 7 days), empyema, necrotizing pneumonia, extrapulmonary infection, harder to treat infections like Legionella, Pseudomonas, MRSA
- Transition to PO when able to oral and clinically stable/improving
- Pediatric: if not immunized against strep and H. influenza, cefotaxime or ceftriaxone.
Corticosteroids
The IDSA guidelines do not suggest routine corticosteroids in CAP, but some studies suggest that you may consider steroids if the patient is severely ill (shock refractory to fluid resuscitation and vasopressor support), (Meijivis, Blum). Steroids have been shown to offer many benefits in those cases, including faster return to clinical stability and shorter length of stay, but no mortality benefit. The main side effects were hyperglycemia. CRP can help stratify the benefit from steroids (CRP >150 mg/L implies a lot of benefit from steroids; a normal CRP should question the pneumonia diagnosis altogether and cast doubt on the benefit from steroids). However, for a patient with a clear diagnosis of severe CAP, don’t delay starting hydrocortisone while waiting for CRP.
The new ATS guidelines state:
- Inpatients with non-severe CAP: Strongly recommend against using systemic corticosteroids (strong recommendation, low-quality evidence).
- Inpatients with severe CAP: Suggest administering systemic corticosteroids (conditional recommendation, low-quality evidence).
Steroids can have a negative impact on mortality in pneumonia caused by influenza (Yang). More studies need to be done in this area.
The guidelines do suggest that steroids can be used in COPD or other disease states that would require steroids.
Directed Therapy
If cultures grow something specific, you can treat just for that and DC any antibiotics that don’t treat (ie: vanc, anti-pseudomonas)
- S. Pneumo: PenG or Amoxil ALT: macrolide, ceph, clinda, doxy, FQ
- Resistant S. Pneumo: cefotaxime, ceftriaxone, Levo ALT: vanc, linezolid, high dose Amoxil
- H. Influenza: Amoxil ALT: FQ, doxy, azithromycin, clarithromycin
- Resistant H. Influenza: 2nd or 3rd gen ceph ALT: FQ, doxy, azithromycin, clarithromycin
- Legionella: FQ, macrolide ALT: Doxy
- MRSA: van, linzesolid ALT: Bactrim
- MSSA: Antistaph PCN (methicillin nafcillin oxacillin cloxacillin dicloxacillin) ALT: cefazolin, clindamycin
- New CAP agents: Omadecycline and Lefamulin: approved for adult CAP. No clinical data for MRSA.
Hospital-Acquired or Ventilator-Associated Pneumonia (HAP/VAP):
HCAP is no longer a category. See CAP.
- Pathogens: Pseudomonas, Acinetobacter, staph, MRSA
- HAP = pneumonia 48 hours admission, VAP= pneumonia 48 hours after ventilation
- Get blood cultures for HAP/VAP. Non-invasive is preferred. Do not diagnose based on procalcitonin. Clinical criteria is more important than biomarkers
- NO AMINOGLYCOSIDE MONOTHERAPY
Treatment:
- In VAP, if the MRSA and Gram Negative Bacterial Resistance (GNBR) rates are <10 or < 20 in HAP: B-lactam only (cefepime, imipenem, meropenem, pip-tazo) OR Levaquin only
- In VAP, if the MRSA/GNBR>10 or >20 in HAP: ADD vanc or linezolid (you can use aztreonam as your beta-lactam or cipro as your FQ in addition to the above)
- High Risk (structural lung disease or IV antibiotics) ADD extra antipseudomonal. Can be above or aminoglycoside (or polymyxins in VAP)
- In VAP, one of the two must have s. aureus coverage
- B-Lactam should have antipseudomonal coverage: ceftazidime, cefepime, imipenem, meropenem, pip/tazo or aztreonam
- Inhaled antibiotics can be used in combo (not alone) in VAP due to Gram – bacilli being susceptible only to AGS or polymyxins
- Avoid polymyxin unless no other choice, Polymyxin B causes less kidney damage than colistin
- Deescalation with cultures or an 80% drop in procalcitonin (this is the best use of procalcitonin in pneumonia – see section below).
- If morbidity risk is high: MRSA and Double Pseudo from 2 classes (Only risk factors are IV antibiotics in last 90 days or structural lung disease). The first agent should be a B-lactam unless contraindicated. B-lactams are almost always preferred in pneumonia.
- High MDR risk factors:
- HAP/VAP:
- Prior IV antibiotic use within 90 days
- VAP Only:
- Septic shock at the time of VAP
- ARDS preceding VAP
- Five or more hospital days prior to VAP occurrence
- Acute renal replace therapy prior to VAP onset
- HAP/VAP:
- Everyone with HAP/VAP needs at least 2 agents. Most patients (patients with MDRs) will need at least 3 according to the guidelines, but those recommendations are based on weak evidence (even according to the guidelines) so double anti-pseudomonal coverage should be individualized.
- ***Linezolid causes thrombocytopenia, check CBC***
- Typically, aminoglycosides should not be used alone for antipseudomonal coverage (true in almost all disease states).
- Treatment Duration: 7 days
Newer Agents
- Ceftolozone-tazobactam: MDR Gram – coverage, including ESBL and AmpC producers, CTX-M, pseudomonas but no activity against carbapenemase producers/CRE, no enterococcus, no anaerobes, NO KPC
- Ceftazidime-avibactam: MDR Gram – including ESBL, AmpC, most CRE, including KPC and OXA-48, limited gram, no STAPH, no pseudomonas, no enterococcus, no anaerobes
- Meropenem-vaborbactam – MDR Gram – including ESBL, AMPC, CRE including KPC, and NON-MDR STAPH
Respiratory Fluoroquinolones
Typically, they’re’ light of of as levofloxacin, moxifloxacin, and gemifloxacin.
What makes them respiratory?
| Cipro (not “respiratory”) | Levo | Moxi | Gemi | |
| Streptococcus pneumoniae | + | +++ | +++ | +++ |
| Pseudomonas aeruginosa | +++ | ++ | + | – |
| Anaerobes | – | – | ++ | – |
| Atypicals | +++ | +++ | +++ | +/- |
Procalcitonin
It is not recommended to start or withhold initial empiric treatment based on procalcitonin alone, however, procalcitonin can be used along with other clinical assessments as evidence that therapy is effective or to de-escalate antibiotics.
| Procalcitonin Guided Therapy | |||
| Procalcitonin Level | |||
| <0.1 ug/L | 0.1-0.25 ug/L | >0.25—0.5 ug/L | > 0.5 ug/L |
| Bacterial infection very unlikely | Bacterial infection unlikely | Bacterial infection likely | Bacterial infection very likely |
| WITHOLD ABX! | Withhold ABX | Start or continue ABX | START or CONTINUE ABX! |
| PCT control after 6-24 h Consider antibiotics if: · Respiratory or hemodynamic instability · Severest comorbidity · Need for ICU admission | PCT control after 6-24 h · Consider antibiotics if · Severe comorbidity · Localized infection (abscess, Empyema) · Compromised host defense (eg immunosuppression, neutropenic ever) · Chronic a/o smoldering infection (e.g. endocarditis, Tbc) | Reevaluation after 3, 5 and 7 days · PCT measurement · Withhold antibiotics using above cut offs | Reevaluation after 3, 5 and 7 days. · PCT measurement · Withhold antibiotics using above cut offs · If initial PCT levels are very high, the withhold when 60-90% decrease of peak PCT |
Self W, et al.. Procalcitonin as a marker of etiology in adults hospitalized with community-acquired pneumonia. Clin Infect Dis. 2018; 66(10): 1640-41.
Schuetz P, et al. Procalcitonin guided antibiotic therapy and hospitalization inpatients with lower respiratory tract infections: a prospective, multicenter, randomized controlled trial. BMC Health Svcs Res 2007;7:102.
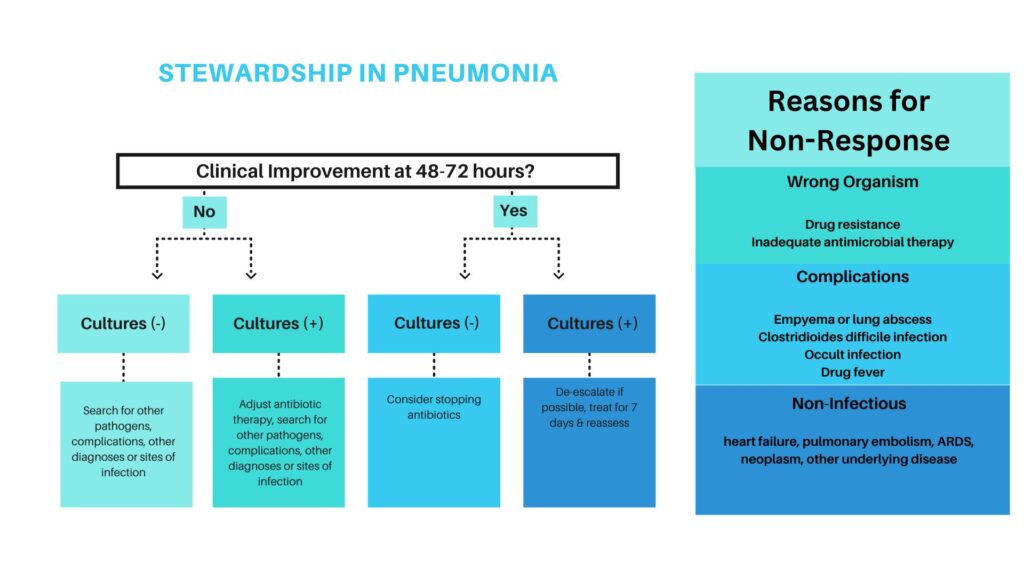
Special Antibiotic Properties:
Anti-Inflammatory Antibiotics:
- Azithromycin famously suppresses inflammation (see Kricker, et al. Nonantimicrobial Actions of Macrolides: Overview and Perspectives for Future Development, Pharmacological Reviews October 1, 2021, 73 (4) 1404-1433) This does help symptom relief in pneumonia and many other conditions.
- Not as famously, fluoroquinolones also suppress inflammation (see Dalhoff A. Immunomodulatory activities of fluoroquinolones. Infection. 2005 Dec;33 Suppl 2:55-70. doi: 10.1007/s15010-005-8209-8.).
Post-antibiotic Effects
The postantibiotic effect (PAE) describes the persistent suppression of bacterial growth after exposure of a microorganism to an antibiotic. The term should not be confused with the effects of bacterial suppression caused by antibiotic subinhibitory concentrations.
Antibiotics that kill bacteria by interfering with protein synthesis usually demonstrate prolonged PAEs (eg, 1–5 hours) against gram-negative bacteria:
- Aminoglycosides
- Clindamycin
- Chloramphenicol
- Macrolides
- Tetracyclines
- Rifampicin
- Quinupristin/dalfopristin (this one is know for it’s post-antibiotic effect )
Antibiotics that kill bacteria by interfering with cell wall synthesis have little, if any, PAE against these types of organisms.
- β-lactams
- Monobactams
- Cephalosporins
- Glycopeptides
The one major exception is the carbapenems (eg, imipenem, meropenem) that exhibit fairly long PAEs against P aeruginosa.
Gram-positive bacteria don’t experience the same kind of post-antibiotic effect (it’s shorter for all antibiotics, ~1 hour).
The clinical relevance of the PAE is related to its use in establishing dosage regimens that are directed against a specific pathogen. It is partially responsible for the success of intermittent dosing with drugs that exhibit short half-lives.
- Drugs with a strong post-antibiotic effect benefit from large intermittent doses because high peak concentrations translate into better post-antibiotic effects.
- Drugs with weak post-antibiotic effects usually must be present at a pivotal point in a microbes reproductive cycle to work. They must be on-board at >MIC at the pivotal point. These drugs usually benefit from continuous or frequent infusions.
The post-antibiotic effect has some relationship to the kill characteristics of the antibiotic, but the relationship is not straightforward. For instance, macrolides are known for time-dependent kill characteristics, but have a strong post-antibiotic effect which probably inhibits bacterial growth rather than causing cell lysis.
F. M. MacKenzie, I. M. Gould, The post-antibiotic effect, Journal of Antimicrobial Chemotherapy, Volume 32, Issue 4, October 1993, Pages 519–537
Sub-MIC Effects
Most antibiotics go below the MIC for longer than the post-antibiotic effect. Sub-MICs have numerous effects on bacteria, including morphological changes, modifications of cell wall structure, altered growth kinetics, inhibition of enzyme or toxin production, and loss of adhesive properties, but these are poorly understood. While some studies have found that exposing bacteria to sub-MICs promotes growth suppression when the bacteria has been previously exposed to supra-MIC concentrations, some studies have found that sub-MICs of oxacillin, methicillin, and amoxicillin promote biofilm formation, possibly even when the bacteria was previously exposed to high MICs.
Tissue Half Life:
Some antibiotics have excellent lung penetration and increased half life in the lungs. Azithromycin demonstrates excellent tissue penetration and intracellular accumulation, especially in the lungs. Following oral administration, azithromycin exhibits rapid intracellular uptake from blood to tissue compartments like the lungs, resulting in tissue concentrations higher than the minimum inhibitory concentration for many pathogens. It is subsequently slowly released back into circulation due to its long terminal phase elimination half-life of ~60 hours, lung concentrations remain therapeutic for up to 98 hours (Baldwin, 1990). Short courses (like “Z-packs”) are appropriate when using azithromycin and similar drugs.
Post-Antibiotic Leukocyte Enhancement:
Bacteria are often more susceptible to phagocytosis after being exposed to antibiotics, even if they’re not killed by the antibiotic.
Sources for Short Courses
Mostly from Brad Spellberg’s Shorter is Better
- Pakistan Multicentre Amoxycillin Short Course Therapy pneumonia study g. Clinical efficacy of 3 days versus 5 days of oral amoxicillin for treatment of childhood pneumonia: a multicentre double-blind trial. Lancet 2002; 360(9336): 835-41.
- Greenberg D, Givon-Lavi N, Sadaka Y, Ben-Shimol S, Bar-Ziv J, Dagan R. Short-course antibiotic treatment for community-acquired alveolar pneumonia in ambulatory children: a double-blind, randomized, placebo-controlled trial. The Pediatric infectious disease journal 2014; 33(2): 136-42.
- el Moussaoui R, de Borgie CA, van den Broek P, et al. Effectiveness of discontinuing antibiotic treatment after three days versus eight days in mild to moderate-severe community acquired pneumonia: randomised, double blind study. Bmj 2006; 332(7554): 1355.
- Uranga A, Espana PP, Bilbao A, et al. Duration of Antibiotic Treatment in Community-Acquired Pneumonia: A Multicenter Randomized Clinical Trial. JAMA internal medicine 2016; 176(9): 1257-65.
- Dinh A, Davido B, Bouchand F, Duran C, Ropers J, Cremieux AC. Honey, I shrunk the antibiotic therapy. Clin Infect Dis 2018; 66(12):1981-2.
- Harris JA, Kolokathis A, Campbell M, Cassell GH, Hammerschlag MR. Safety and efficacy of azithromycin in the treatment of community-acquired pneumonia in children. The Pediatric infectious disease journal 1998; 17(10): 865-71.
- Ginsburg AS, Mvalo T, Nkwopara E. et al. Amoxicillin for 3 or 5 Days for Chest-Indrawing Pneumonia in Malawian Children. NEJM. 2020 383: 13-23.
- Dinh A, Ropers J, Duran C, et al. Discontinuing β-lactam treatment after 3 days for patients with community-acquired pneumonia in non-critical care wards (PTC): a double-blind, randomised, placebo-controlled, non-inferiority trial. Lancet. 2021 397:1195-1203.
- Bielicki J, Stohr W, Barratt S, et al. Effect of Amoxicillin Dose and Treatment Duration on the Need for Antibiotic Re-treatment in Children With Community-Acquired Pneumonia. The CAP-IT Randomized Clinical Trial. JAMA. 2021;326(17):1713-1724.
- Williams DJ, Creech CB, Walter EB, et al. Short- vs. Standard-Course Outpatient Antibiotic Therapy for Community-Acquired Pneumonia in Children. JAMA Pediatrics. 2022. 176(3):253-261.
- McCallum G, Fong S, Grimwood K, et al. Extended Versus Standard Antibiotic Course Duration in Children <5 Years of Age Hospitalized With Community-acquired Pneumonia in High-risk Settings: Four-week Outcomes of a Multicenter, Double-blind, Parallel, Superiority Randomized Controlled Trial. Ped Infect Dis J. 2022. 41(7):549-555.
- Chastre J, Wolff M, Fagon JY, et al. Comparison of 8 vs 15 days of antibiotic therapy for ventilator-associated pneumonia in adults: a randomized trial. JAMA : the journal of the American Medical Association 2003; 290(19): 2588-98.
- Capellier G, Mockly H, Charpentier C, et al. Early-onset ventilator-associated pneumonia in adults randomized clinical trial: comparison of 8 versus 15 days of antibiotic treatment. PLoS One 2012; 7(8): e41290.
- Mo Y, Booraphun S, Li AY, et al. Individualised, short-course antibiotic treatment versus usual long-course treatment for ventilator-associated pneumonia (REGARD-VAP): a multicentre, individually randomised, open-label, non-inferiority trial. Lancet Resp Med. 2024. ePub.
