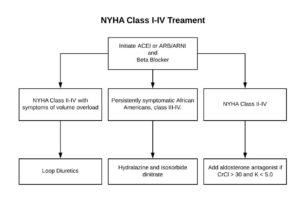
Stages of CHF: Stages of CHF NYHA Functional Class A High risk of heart failure but no structural disease or symptoms. none B Structural heart disease but without signs or symptoms of HF. I Asymptomatic HF. No limitations in physical activity caused by HF symptoms. C Structural heart disease with prior or current symptoms of […]
heart failure
Beta-Blockers
B1 Selective Blockers Non-Selective Blockers (B1 and B2) Mixed Blockers (Beta and alpha) Hydrophilic acebutolol, atenolol, bisoprolol (both), esmolol nadolol, pindolol, sotalol Lipophilic bisoprolol (both), metoprolol, nebivolol propranolol carvedilol, labetalol Some points: Avoid mixed and non-selective agents in asthma. Alpha blockade causes vasodilation, decreases peripheral resistance, and causes no reflex tachycardia. (acronym: Can Let No […]