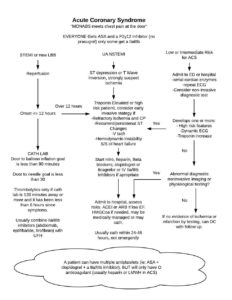
Anticoagulant Overview: STEMI, PPCI UHF, bivalirudin STEMI, fibrinolytic UHF, enoxaparin, fondaparinux bivalirudin not studies with lytics NSTE-ACS, early invasive enoxaparin, bivalirudin, fondaparinux, UFH if you’re going to cath lab, allif placing a stent, no fondaparinux NSTE-ACS, ischemia-guided enoxaparin, fondaparinux, UFH Stop heparin after the intervention. Everyone with ACS gets dual anti-platelets for 12 […]